Guardian Angel
The AngelEye Blog
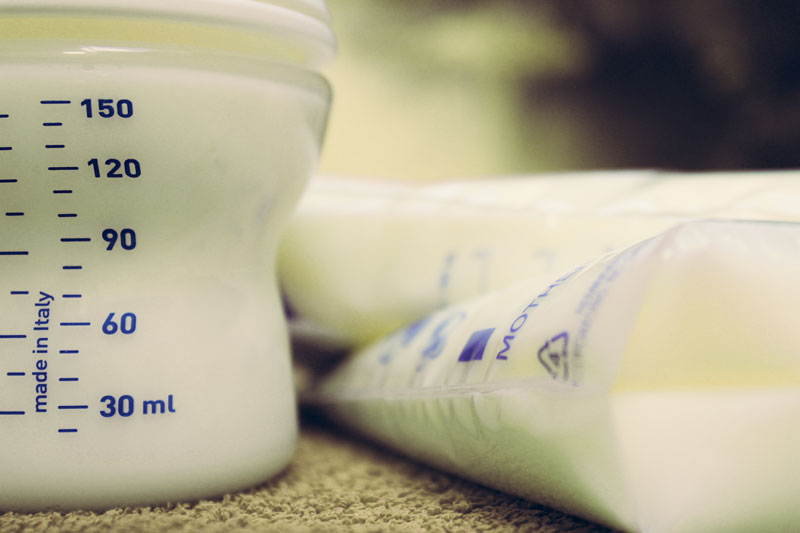
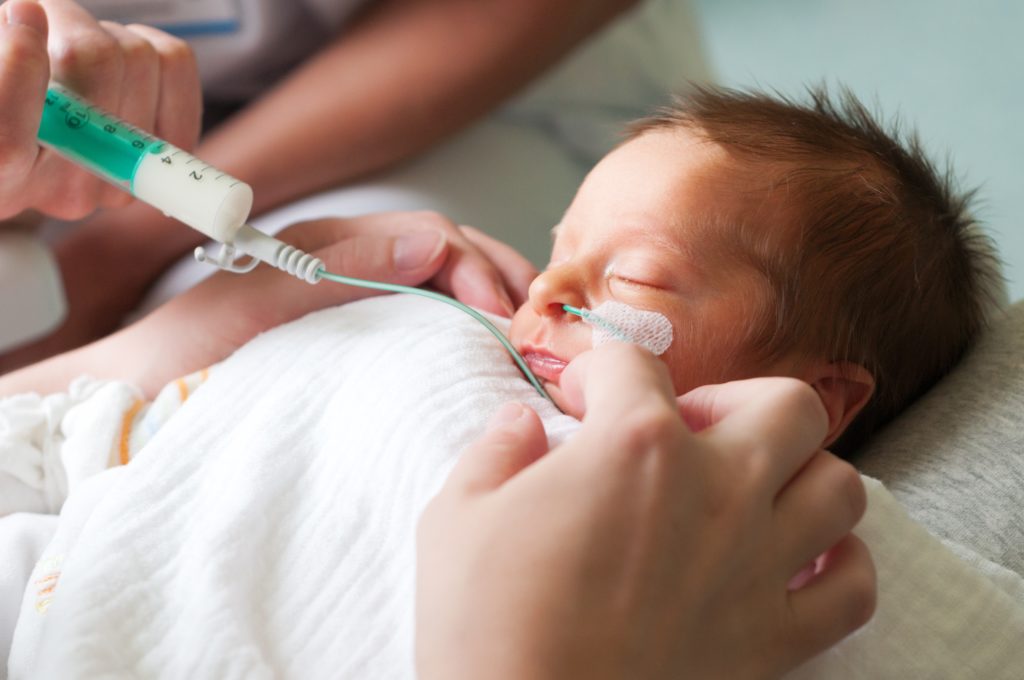
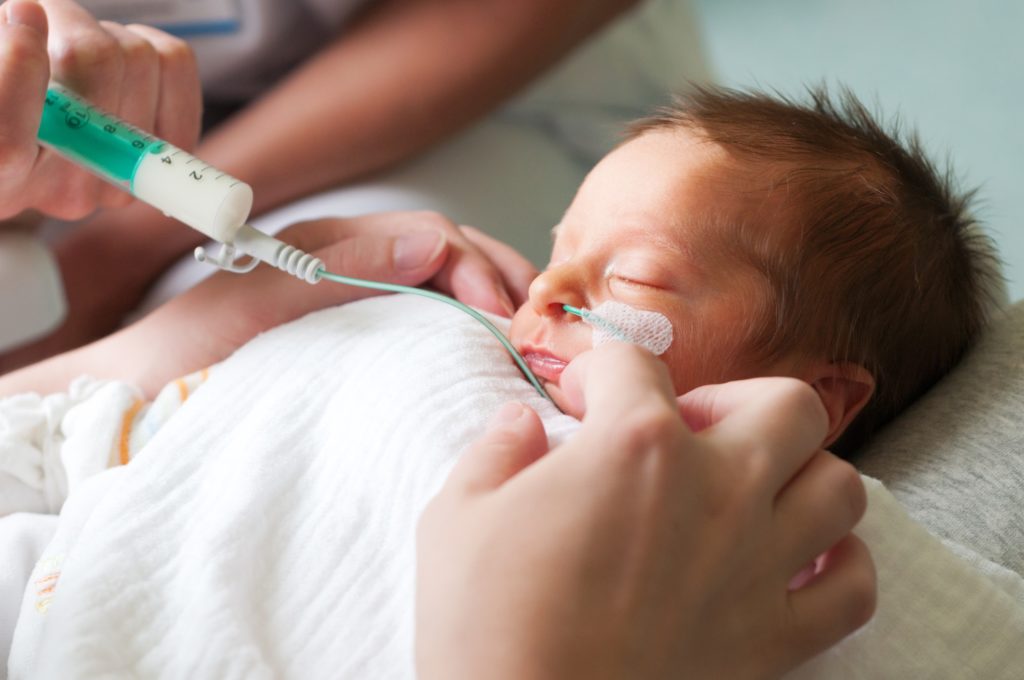
Breastfeeding Can Look Different on Everyone
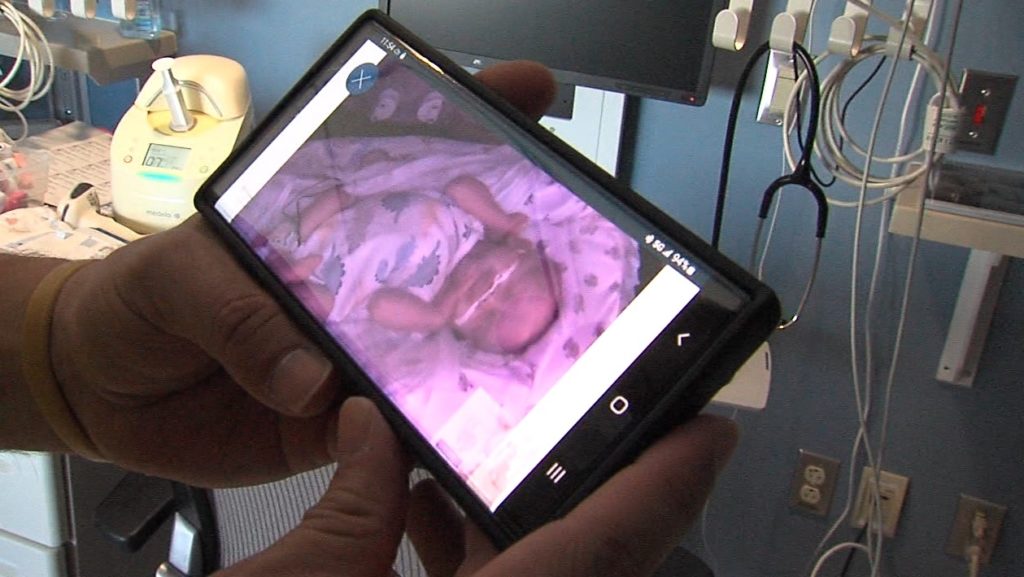
Celebrating Lactation in the NICU. World Breastfeeding Week and National Breastfeeding Month in August gave us reasons to elevate the conversation about breastfeeding and mothers’ own milk as key ingredients for healthy infants and children.