Prematurity Awareness Month: Honoring Norah Marie Wilson
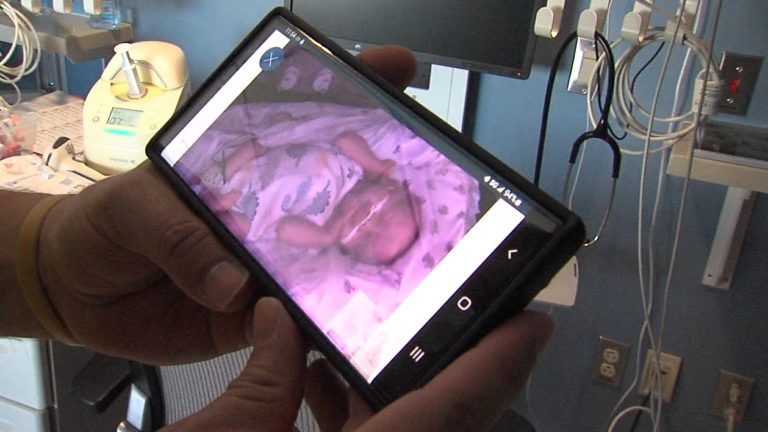
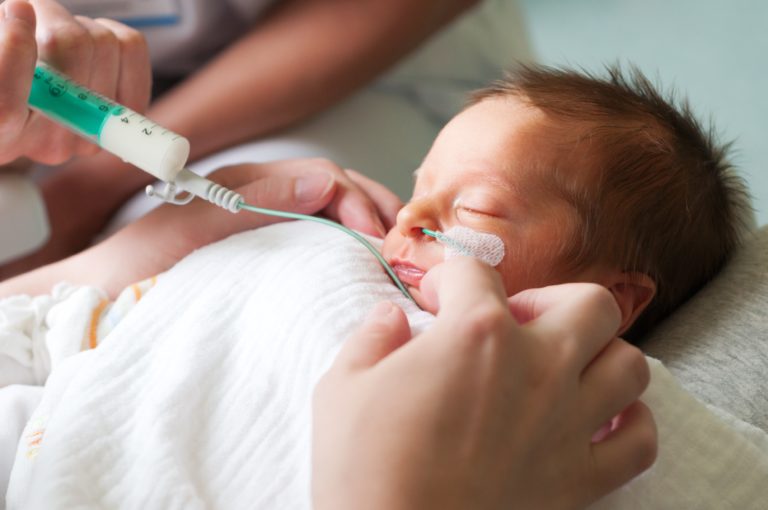
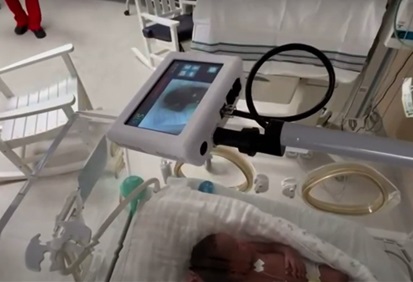
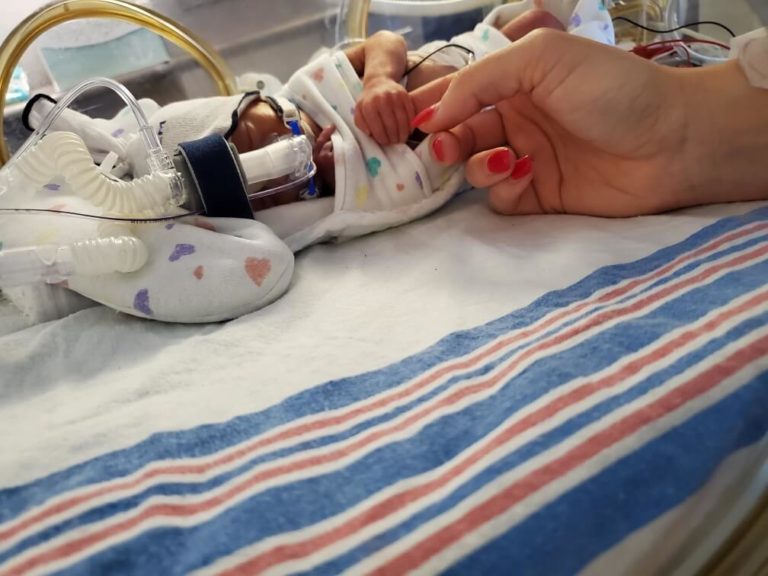
Premature births take many journeys that are highlighted during Prematurity Awareness Month. While thousands of NICU babies successfully transition home to their families every year, it’s important to honor the little ones lost during their hospital stay. This year we highlight Norah Marie Wilson and the Norah Foundation’s Always Together project – the effort that brought the first NICU cameras to Northern California.